The first new retinoid molecule approved in over 20 years is now available in Canada.
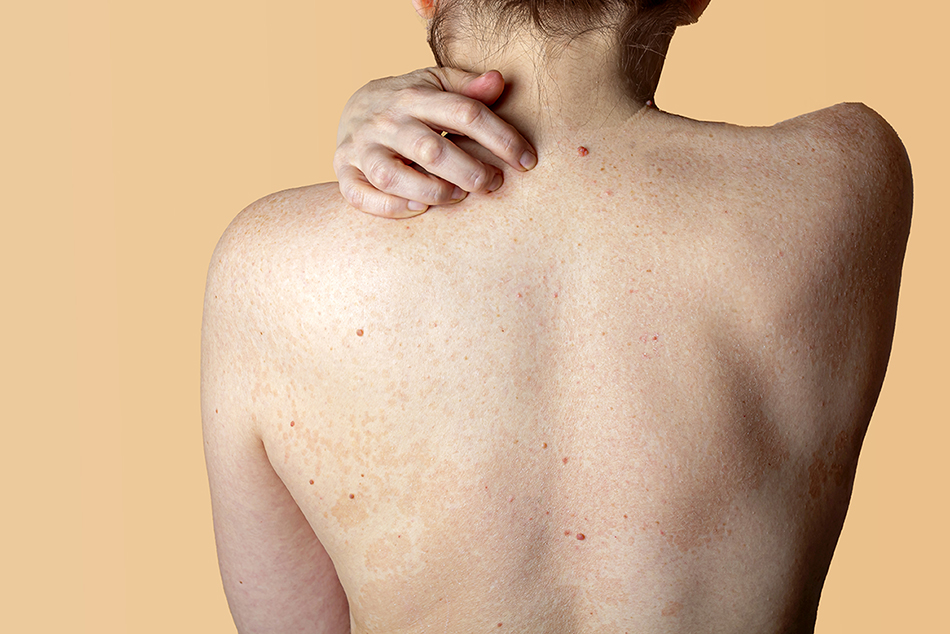
Sudden breakouts – an unexpected outcome of living through the COVID-19 pandemic – aren’t limited to your face. Trunk acne, which refers to acne on the back, shoulders and chest, affects approximately 52 percent of people who have facial acne, and is becoming increasingly common as we spend more time at home.
“We’ve certainly got acne flare ups around the mouth from wearing masks,” says Dr. Benjamin Barankin, dermatologist and medical director at the Toronto Dermatology Centre. With a dark, warm and humid environment comes increased inflammation and bacterial overgrowth, inviting “maskne” (mask + acne) – the term referring to the unsavoury consequence of preventative mask-wearing – into our vocabulary.
The same idea applies to our bodies. “As far as trunk acne, it’s possibly worse just from occlusion. If we’re sitting at a chair doing work from home and Zooming, we’re not getting up and around as much,” says Barankin. In addition to reduced movement, lack of sleep and increased stress levels are leading to a decline in the quality of our skin beyond our face. “There’s a lot of stress related to COVID, whether people realize it or if it’s subclinical, it’s there.”
Trunk acne is generally harder to treat than face acne, according to Barankin. Though it’s less visible, it tends to be more inflammatory, as the skin is thicker and oil glands are deeper. It’s also worth mentioning that we tend to pay less attention to our backs and chests when cleansing. “We’re not seeing it every day so it’s not top of mind,” he says. “We also know that a little bit of sunlight helps acne, and you’re more likely to get that on your face than on your trunk.” Consequently, those with trunk acne are more likely to seek a prescription in order to effectively treat it. “We often forget that it’s not just that it doesn’t look good,” says Barankin. “A surprising amount of suffering that occurs with acne even though it’s not a deadly condition, so to speak. It’s a visible condition. If you have high blood pressure or high cholesterol, nobody knows. You can keep that to yourself. When you have acne, the whole world sees it.”
Enter Akleif, the first prescription body medication to be specifically studied for trunk acne and the newest generation of topical retinoids. “It specifically targets the retinoic acid receptor gamma, which is the most common retinoic acid receptor found in the skin,” says Barankin. “I think the reason that we’re seeing nice results with this product is that you’re covering more areas of the skin that are going to be responsive to this product than to other retinoids because there’s more receptors there to bind this product.”
“This new approval marks an important milestone in effectively treating acne in Canada, especially truncal acne,” says Dr. Melinda Gooderham, a dermatologist and Medical Director at the SKiN Centre for Dermatology and the SKiN Research Centre in Peterborough, Ontario. “The clinical evidence demonstrates that Akleif reduces inflammatory lesions on the face, back and chest while delivering low systemic levels. This ensures efficacy, safety and tolerability which makes Akleif particularly useful for the treatment of acne lesions that appear on large surfaces of the skin, like the back and chest of some acne patients.”
When should you consider a prescription to treat acne? “When the acne is mild and early on, start treating it using a gentle cleanser and moisturizer, along with over-the-counter products that have things like salicylic acid, benzoyl peroxide and glycolic acid,” says Barankin. “If you’re finding after three months or so of doing that, that you’re seeing scarring, or the acne is affecting you psychologically – like it’s affecting how you dress whether you’re going out or seeing friends – then definitely you want to come on in and see your physician and consider prescription therapy.”
Credit: Melissa Perdigao, ellecanada.com
