A plastic surgeon (look for MD FRCSC), like a dermatologist (look for MD FRCPC), has a minimum of 5 years of extra training after receiving a medical degree (typically 4 years).
Our state-of-the-art facility has been designed to provide you with the best available technology and expertise to ensure your comfort and confidence in the care that you will receive at Toronto Dermatology Centre. Our board certified, credentialed and experienced plastic surgeon has performed thousands of successful surgical procedures.
Plastic Surgeon
Dr. Robert Backstein has been practicing Plastic and Reconstructive Surgery with Royal College of Canada certification since 1999. He attended the University of Toronto for his undergraduate medical degree and completed a five-year Plastic and Reconstructive Surgery Residency at the University of Toronto. Dr. Backstein has extensive experience in both cosmetic plastic surgery, and non-cosmetic plastic and reconstructive cases.
Dr. Robert Backstein has always had a special interest in plastic surgery pertaining to the skin – benign, pre-malignant, and malignant lesions, scar surgery, keloids and other aspects of skin-related plastic surgery. He undertook a three month selective in dermatopathology under Dr. Lynn Fromm, a world-renowned expert in melanoma during his Plastic Surgery Residency training program at the University of Toronto. Dr. Backstein’s practice has focused increasingly on the surgical management of skin lesions. This separates Dr. Robert Backstein from most other plastic surgeons who treat these conditions as part of a practice that focuses primarily on other areas of care. Dr. Backstein has been the Director of Plastic Surgery Services at the Toronto Dermatology Centre (TDC), one of the largest & busiest dermatology clinics in Canada since 2011. Dr. Backstein has a special interest in techniques to minimize scarring, and administration of local anesthesia injection in the most comfortable manner possible.
Dr. Backstein prides himself on offering a wide range of surgical and non-surgical options for enhancing our clients’ appearance and well-being, as well as dealing with potentially serious medical conditions such as skin cancers.
Our plastic surgeon Dr. Robert Backstein provides both OHIP and non-OHIP procedures including:
- Mole, cyst, lipoma and blemish removal
- Skin cancer surgery (basal cell cancer, squamous cell cancer, melanoma)
- Scar revision
- Ear lobe repair
For more details please call: 416-633-0001 ext. 0 or email: [email protected]
Before & After Removal
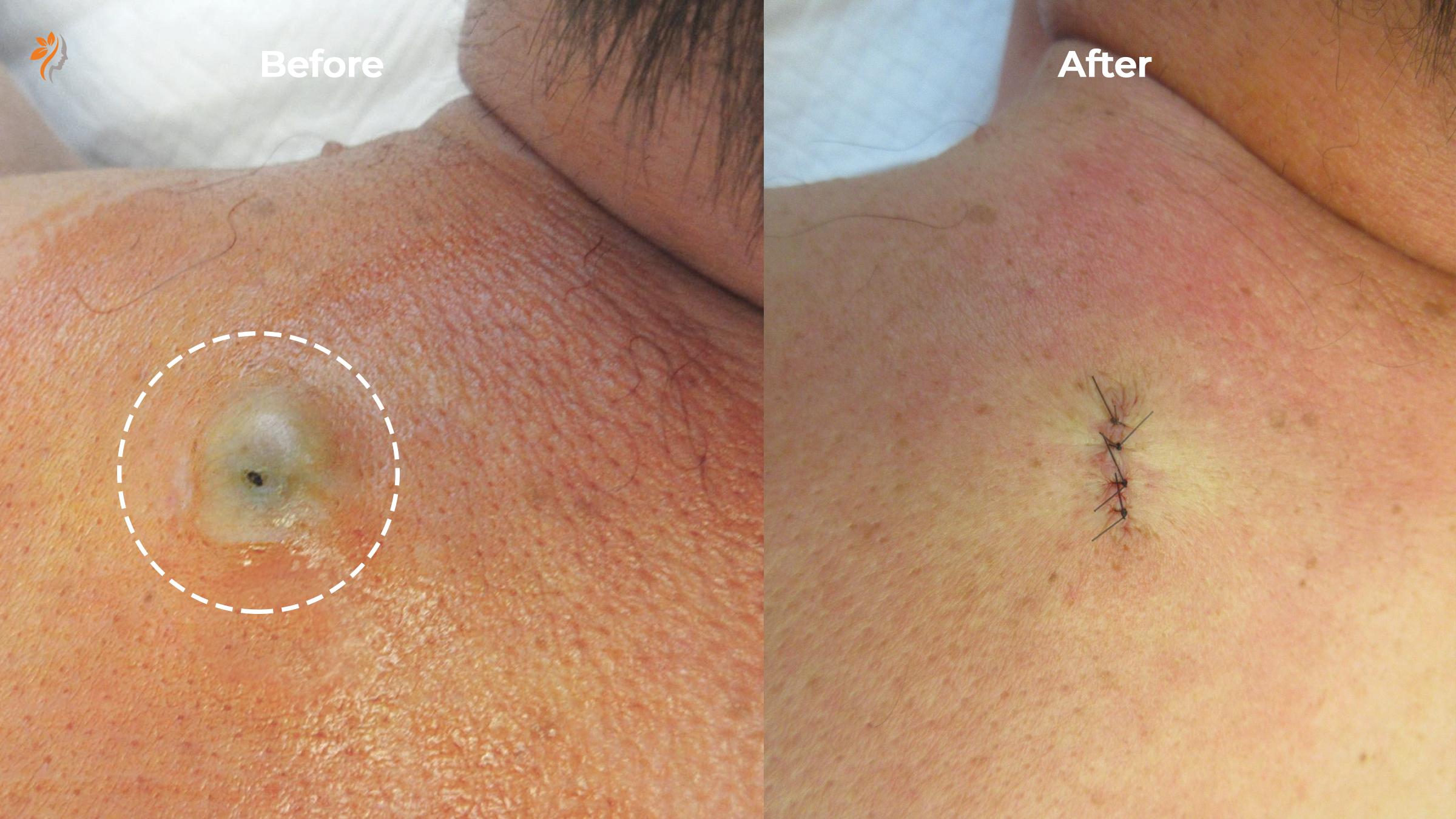
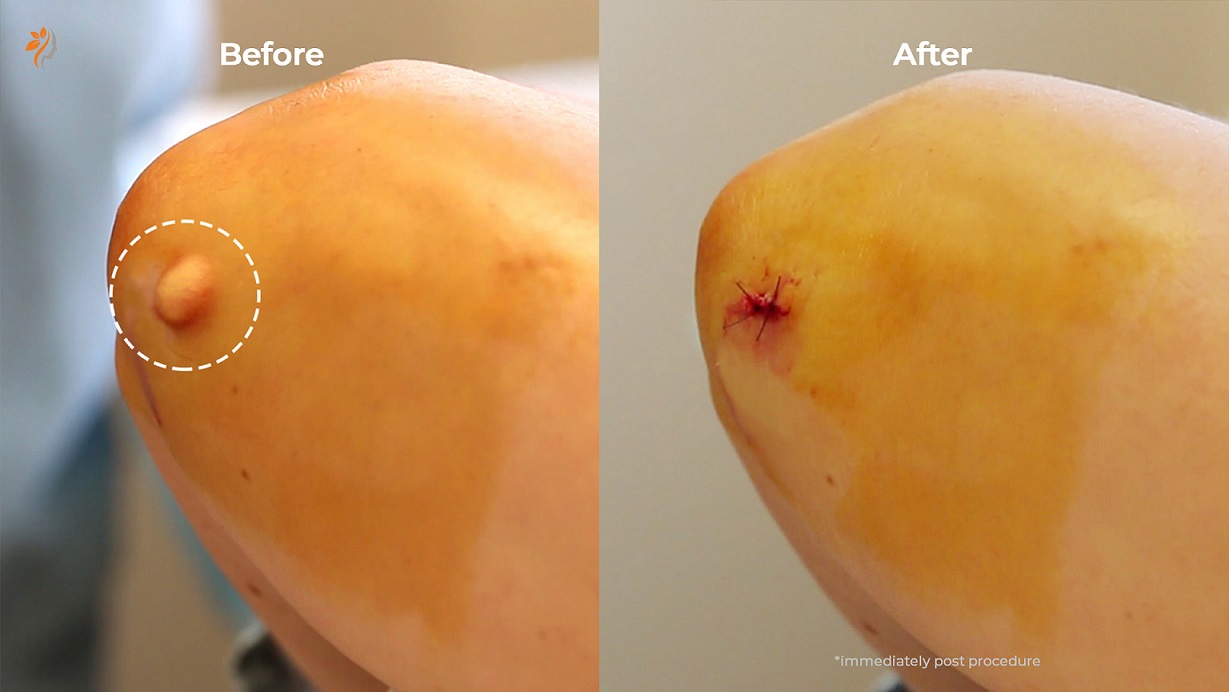
The Minor Surgery Process
Surgical procedures performed at Toronto Dermatology Centre (TDC) are all performed under local anesthesia (a “freezing” needle, similar to what a dentist uses to numb the teeth). If you have a history of allergy or reaction to local anesthesia, be sure to make a staff member aware prior to arrival for your procedure. Sedations and general anesthesia are not administered during the process so the early recovery is much easier. There is generally no need to stop medications and there is no requirement to fast or refrain from drinking before your procedure.
Minor surgery begins with Dr. Backstein preparing the surgical site with an antiseptic solution and then administering the local anesthesia. Dr. Backstein takes pride in having paid a great deal of attention over his years of practice to refining his technique of local anesthesia injection so as to minimize the discomfort felt with the needle and injection process.
Once the area is totally numb and anaesthetized (meaning no more pain/discomfort during the procedure), the surgical procedure is carried out. Stitches are used where deemed necessary and appropriate for optimal healing. Having spent many years performing major cosmetic plastic surgery procedures, Dr. Backstein has extensive experience in surgical techniques that optimize and minimize scarring as well as the best methods of stitching incisions in order to achieve the best possible aesthetic results.
Once the procedure is complete, bandages are applied by a medical assistant staff member, and the patient is then ready to leave the office. Wound care and instructions for home care are reviewed by the medical assistant and a handout is given to all patients that reviews the instructions discussed.
Frequently Asked Questions
Surgical stitches can be classified as absorbable (dissolving) or non-absorbable. Absorbable stitches dissolve, usually by means of enzymes found in the tissues, and therefore, do not need to be removed.
Non-absorbable stitches do not dissolve and need to be removed, usually 1-2 weeks after surgery. Generally, absorbable stitches are used to stitch deep layers below the skin. They can also be used to close the top skin layer and many patients request this, assuming it’s a better and more convenient choice since they will not need to return for a stitch removal appointment.
In many cases, however, a non-absorbable suture is a better choice for skin closure especially in cosmetically important areas such as the face because the process of stitch absorption might lead to extra inflammation and even more visible scars, particularly in the short run. Also, absorbable stitches may not be the best choice in high stress body areas such as the shoulder or back since they are less durable and more prone to breaking before the incision has healed completely leading to the wound opening.
There are definitely exceptions to the above guidelines. Dr. Backstein will always suggest the best option for your particular case.
Stitch removal timing is a very common question after minor surgery.
Facial and neck sutures are generally removed around 7 days; other areas at 10-14 days. Keep in mind that this is a very general guideline and Dr. Backstein will look at each case individually.
For example, if larger lesions are removed from the skin, a larger “defect” is temporarily created during surgery so the tightness or “tension” on the stitch closure is greater because the skin has to be stretched over a wider gap to be closed with stitching. As such, removing the sutures somewhat later than the guidelines above might be called for to ensure that the wound doesn’t begin to separate and open up after the stitches are taken out.
Also, procedures done on areas with a lot of movement such as around the elbow, knee or low back might involve removal of stitches a few days later than usual. In these cases, letting the incision heal more thoroughly prior to stitch removal might be called for.
One of the most common questions patients ask after minor surgery is when they can resume exercising after minor surgery. There are a couple of issues at play with this. Dr. Backstein generally recommends keeping the the surgical site dry for 36-48 hours to prevent water entering the incision or softening of stitches. This will be difficult or impossible to adhere to with heavy sweating or subsequent showering associated with exercising.
Even more important, however, is the risk of disrupting your stitches by stressing the surgical site too heavily when exercising. Dr. Backstein’s best advice is to stay away from heavy exercise for a week to 10 days or until your stitches are removed and healing reassessed by the medical staff at TDC.
If you are going to exercise sooner, make sure to take it slow and focus on activities that do not put heavy stress loads on the body area that was operated on. Remember that if you insist on exercising before the recommended time has passed, you are doing so at your own risk of the wound opening up which can lead to a much slower healing process and poorer scar quality.
This is another common question and concern from patients undergoing minor surgery at TDC. Different surgeons may have slightly different answers, but Dr. Backstein’s recommendation is to not stop any medications prior to your procedure.
The main medications in question are blood-thinning drugs such as: Aspirin, Advil, Coumadin, Xarelto, etc. Dr. Backstein’s feeling, which is also supported by clinical studies looking into this very question, is that stopping these medications is not necessary to ensure safe and uncomplicated surgery and may, in fact, put patients at risk for thromboembolic events such as stroke, blood clots, or heart attack while they are off their medications.
In minor surgeries, bleeding can be very easily controlled using electrocautery, sutures and bandages.
In summary, Dr. Backstein suggests patients continue all of their usual medications without interruption.
Understanding the healing process is one of the most important things patients can do to take the stress out of the notion of having a scar created on their body from surgery. This is truly a situation for which knowing what to expect is of utmost importance.
Dr. Backstein explains wound healing and scarring to patients as a process that has two phases. The first phase is referred to by Dr. Backstein as the “angry phase” of wound healing. During this early period that lasts about 2 months, your body is simply trying to mend the incision in a way that leads to a healed cut with no infection and adequate durability. During this early phase, you can expect the scar to actually become somewhat more noticeable, redder, and “angrier” looking every week. Make-up and concealer can easily be used to hide these features of your scar once the go ahead is given by the medical staff.
It is only after this first phase of healing that the process of scar fading, flattening and general aesthetic improvement of your scar will begin to happen and the final scar appearance and quality will really not be evident until 12-24 months after the procedure was done. This does not mean that it will take that long for you to be comfortable with the appearance of the scar, but that the scar will continue to improve over that period of time. So be patient, don’t judge your results too early on, and never seek interventions for your scar until at least one year after your surgery when your body has had an adequate chance to complete the healing process.
Treatment of sub-optimal scars is a complex topic. There is no single recipe for success and it all depends on what specific features are making the scar look unsatisfactory. For example, a thicker raised scar (hypertrophic or keloid scar) may benefit from silicone treatments and/or cortisone injections while a scar that is hyper-pigmented (too dark relative to the surrounding skin) may do well with special creams or laser depigmentation treatments. Some scars may be good candidates for surgical scar revisions especially if something very specific went wrong with the healing process (such as infection or wound opening) that, if avoided the second time around, may very well allow a much better scar to form.
Leading up to their surgical procedure at TDC, many patients ask Dr. Backstein if he will do “plastic surgery” if their scar turns out to show more than they had hoped. It is important to understand that Dr. Backstein uses all the best techniques of plastic and cosmetic surgery in all of his minor surgery procedures so the first procedure itself is done using “plastic surgery” in order to optimize scar quality. As such, if a scar turns out to be unsatisfactory, it is not because best techniques were not used the first time around. Having said that, surgical revisions can be useful in specific cases as outlined above.
Patients must keep in mind that all surgical procedures produce scarring. Dr. Backstein will use the best and most meticulous techniques to allow all patients the opportunity to form the best scars that their particular skin can create but nothing can ever be guaranteed because we all heal differently.
When a skin cancer or pre-cancer is removed, the tissue removed is always sent to the lab for a biopsy (typically it takes 10-14 days for the results). The biopsy report provides Dr. Backstein with two important pieces of information: the diagnosis and an assessment of surgical margins.
Surgical margins refer to the edges and underside of the piece of tissue removed by Dr. Backstein and sent to the lab for analysis. Specifically, we are interested in whether or not the cells that are abnormal (cancerous or pre-cancerous) are seen at the very edges or underside of the tissue. If so, a second surgical procedure is generally needed to remove more tissue from around the same site on the body where the first procedure was performed in order to ensure that the lesion is completely removed and that the risk of recurrence or even spread is eliminated. It is important to keep in mind that in these cases of what is called a “positive margin”, Dr. Backstein didn’t neglect or forget to remove all of the necessary tissue. These missed parts are absolutely invisible to the human eye and only visible at the laboratory where very high power microscopes and special tissue-staining techniques are used to identify that further surgery is needed to completely remove the growth. So, what is seen as the edge or extent of the growth in the clinic at TDC and where the edge of the lesion actually is can be two very different things. This creates a bit of a conundrum for plastic surgeons when removing skin growths, especially on cosmetically sensitive areas such as the face. Dr. Backstein always aims to remove the entirety of what is necessary the first time around, but also doesn’t want to “overshoot” the size of the excision in order to ensure he has captured the invisible components because that would lead to unnecessarily large scars being created.
If you are asked to return to the clinic for a second procedure for positive margins, you can expect the procedure to be nearly identical to the first procedure. In most cases, Dr. Backstein will be removing in the realm of millimetres (not centimetres) of additional skin in order to complete the removal of the growth.
Pain is one of the most subjective and individualized elements of recovery from minor surgery performed at TDC. In general, surgical sites are not painful but are tender, i.e. the area is uncomfortable if pressed on or inadvertently touched but generally not bothersome otherwise. In the vast majority of cases, no pain medication prescription is needed and all that is needed is Advil (ibuprofen) or Extra-Strength Tylenol or most commonly, nothing at all.
There are definitely exceptions to this, mostly when specific body areas are operated on. The most sensitive areas are the hand, foot, ear, and scalp in Dr. Backstein’s experience. Also, excision of larger lesions leaves a larger skin defect that needs to be closed with stitches such that the “tension” or pulling on the skin to close it with stitches is greater and this can definitely lead to greater post-operative pain. In these cases, pain generally subsides greatly after about 48 hours but Dr. Backstein will provide a prescription for a stronger pain killer such as Tylenol #3 that patients can take or not take at their own discretion.
Treatment of most benign lesions are considered unessential services by the Ministry of Health and are not covered by OHIP. These benign growths and lesions include: cysts, lipomas, non-suspicious moles, vascular growths, fibromas (e.g. dermatofibromas), skin tags, cholesterol deposits (xanthelasma), warts and others.
It is important to understand that coverage by OHIP is exclusively determined by the Ministry of Health, and is not up to the discretion of Dr. Backstein or your family physician. The size of the growth, and whether it is causing discomfort generally does not influence OHIP coverage. For example, a lipoma or cyst that has been left long enough to grow to the point of causing discomfort, does not shift the procedure into the OHIP-covered category as that would favour patients who have left lesions on their bodies to grow for a long time and put at a disadvantage patients that choose to have similar lesions excised early on.
Before scheduling your appointment, you’ll be asked to send a few pictures of the area of concern. Our surgeon will review and provide a quote if this skin concern is deemed cosmetic or advise if it’s not covered by OHIP. Please note all non-OHIP procedure must be prepaid in full upon booking.
Wound Care Instructions After Skin Biopsy or Surgery
Toronto Dermatology Centre is located in Toronto, Ontario, and serves men and women in North York, Vaughan, Richmond Hill, York, Aurora, Thornhill, Mississauga, Etobicoke, Scarborough, Pickering, Peterborough, Guelph, Kitchener, Waterloo, Hamilton, Oshawa, Barrie, downtown, midtown, uptown and all of Greater Toronto (GTA).
Thinking of visiting Toronto’s premier skin clinic soon?
Fill out the inquiry form below and let us know your area of interest.
Call us today @ 416.633.0001
