The Toronto Dermatology Centre is one of the top places in Canada to manage your mycosis fungoides (MF). Our staff of outstanding dermatologists offer both a comprehensive assessment and diagnosis of your skin, and also discuss all the treatment options such as creams, etc.
 What is Mycosis Fungoides or Cutaneous T-Cell Lymphoma?
What is Mycosis Fungoides or Cutaneous T-Cell Lymphoma?
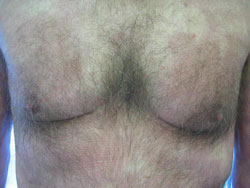
Mycosis fungoides (MF) is a type of cancer of the T-lymphocytes (white blood cells) that affects the skin and the blood. Occasionally, it also involves the lymph nodes and internal organs. The malignant T-cells are attracted to the skin and can appear anywhere on the body surface. If it is mild, there will only be a rash, but if it is more severe, thick lesions called tumors can form. In some instances the skin becomes red all over.
What is the Progression of MF?
The course of MF can be unpredictable. Some patients progress slowly, rapidly, or not at all. Most patients will only experience skin symptoms without serious complications. About 10% of people diagnosed with MF will experience a progression with lymph node, internal involvement, or serious complications. Most patients live normal lives while they treat their disease, and some are able to remain in remission for long periods of time.
Causes of MF
MF is a rare disease and the cause remains unknown, but research continues. MF is not contagious and is not inherited. It is more common after the age of 50.
What is the Course of MF?
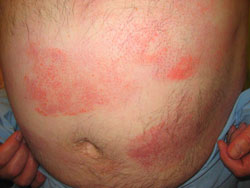
Generally it has a slow course and often remains confined to the skin. Mycosis fungoides has three phases: patch, plaque, and tumor. The patient may have one or all of these phases which can appear anywhere on the skin. Patches are usually flat, red, and scaly. They are often mistaken for eczema or dermatitis because often patients will complain of itching. Plaques are thicker raised lesions. Tumors are larger lesions that can ulcerate and can become huge and mushroom shaped (fungoides). The disease is not a fungal infection.
Is There a Cure?
While there is no cure, research is ongoing. Patients diagnosed early (disease involving less than 10% of the body) can live a normal life expectancy.
Diagnosis
MF is not an easy disease to diagnose. It may take years to make a diagnosis. Dermatologists diagnose MF from the patient’s medical history, performing a physical examination, and obtaining blood tests and skin biopsies. Many skin biopsies may be needed in order to make the correct diagnosis.
Treatment
The goal of t cell lyphoma treatment is to control symptoms such as itching and burning, and to make the patches and skin tumors go away. T cell lymphoma reatment is based on the type of MF, patient’s health, extent of disease, age, and lifestyle. Different treatments include: application of creams and ointments to the skin, oral medication, light therapies, interferon injections, and radiation.
 Topical creams
Topical creams
Cortisone (Corticosteroid) Cream – Cortisone is a drug that reduces inflammation. Cortisone creams temporarily control skin inflammation in many patients with MF and is often the first treatment of choice. Generally, lower strength cortisone preparations are used on sensitive areas of the body such as the groin, armpits, and face. Stronger preparations are usually needed to control affected skin elsewhere on the body. Side effects of the stronger cortisone preparations include: thinning of the skin, dilated blood vessels, bruising, and skin color changes. If creams are stopped too quickly the disease may get worse. MF may become resistant to cortisone creams with time.
Nitrogen Mustard – Nitrogen mustard ointment and liquid is a type of topical chemotherapy that may clear the skin temporarily and control MF. Patients use gloves to apply nitrogen mustard once daily. The face, groin, and armpits are sensitive; patients should ask their dermatologist whether these areas should be avoided. A possible side effect may be an allergic reaction to nitrogen mustard, which involves skin irritation. This treatment is currently difficult to access in Canada.
Imiquimod (Aldara) – Imiquimod is a topical immune response modifier that has been shown to be effective in some patients with mycosis fungoides.
Light Therapies
PUVA or Ultraviolet Light B (UVB) or Narrow-Band UVB Ultraviolet Light – slows the rapid growth of skin cells and is safe and effective under a doctor’s care. Light boxes are used to deliver ultraviolet rays that can treat MF. Treatments are 2-3 times/week and can take several months.
Oral
Corticosteroids – This is a group of drugs that have powerful anti-inflammatory properties. Corticosteroids (prednisone) is usually used in severe cases of MF. It can be used alone or in combination with other treatments.
Methotrexate – This is an oral anticancer drug that is used to control MF. Side effects include upset stomach, nausea, mouth ulcers, and dizziness. Liver function is monitored as well.
Systemic Chemotherapy
These medications kill cancer cells intravenously. Chemotherapy given in this way is called systemic treatment because the drug enters the bloodstream and travels through the body killing cancer cells.
X-ray Therapy
Spot radiation is sometimes used to focus on the affected area in the skin in an effort to kill cancerous cells. Another type of radiation is directed at the whole body called total body irradiation or TSEB.
Interferon
This medication is used to control tumor growth. It is given by injection under the skin 3-5 times a week. Injections can be given by the patients themselves, a person at home, or by a dermatologist.
