The Toronto Dermatology Centre is one of the top places in Canada to manage your acne. Our staff of top-notch dermatologists can offer both a comprehensive assessment and diagnosis of your skin, and also discuss all the treatment options including: prescription creams, prescription pills and over the counter treatments.
What is Lichen Planus
Lichen planus (LP) is an inflammatory disease that affects the skin, the mouth (oral), or both. It may also affect the genital skin, scalp, and nails. LP occurs most frequently in middle-aged adults. The cause of LP is not known. While there are many theories to explain LP, most dermatologists believe it can be classified as an autoimmune disease. There are cases of lichen planus-type rashes that occur as allergic reactions to medications for high blood pressure, heart disease, and arthritis. Identifying and stopping the drug helps clear up the condition within a few weeks. Some people with erosive lichen planus in the mouth can also have hepatitis C, and the dermatologist may check for it.
What Lichen Planus is Not
LP is not an infectious disease. It is impossible to catch LP from someone or to give it to someone else. The disease is not a form of cancer, it does not appear to be inherited, and it is not related to diet.
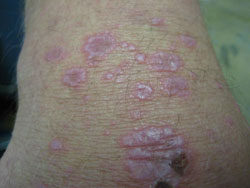
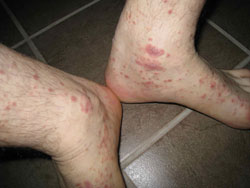
Lichen Planus of the Skin
LP of the skin is characterized by reddish-purple, flat-topped bumps that may be very itchy. Some may have a white lacy appearance called Wickham’s striae. They can be anywhere on the body, but seem to favor the inside of the wrists and ankles. The disease can also occur on the lower back, neck, legs, genitals, and in rare cases, the scalp and nails. LP on the legs is usually much darker in appearance. There may be thick patches (hypertrophic LP) especially on the shins. Blisters are rare. While the typical appearance of LP makes the disease somewhat easy to identify, a skin biopsy may be needed to confirm the diagnosis.
LP of the skin usually causes few problems and needs no treatment. If there is severe itching there is help. Many cases of LP go away within two years. As it heals, LP often leaves a dark brown discoloration on the skin. Like the bumps themselves, these stains may eventually fade with time without treatment. About 20% of people will have a second attack of LP.
Treatment for LP of the Skin
There is no known cure for LP, but treatment is often effective in relieving itching and in improving the appearance of the rash until it goes away. Since every case of LP is different, no one treatment is perfect. The most common treatment is the use of topical corticosteroid creams. More severe cases of LP may require stronger medications such as cortisone taken by mouth, oral retinoids (e.g. Soriatane, Accutane), oral metronidazole antibiotic. Discuss any potential drug side effects with your dermatologist. Since new areas of LP can form in any damaged skin, try to avoid injury.
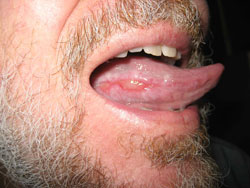
Lichen Planus of the Mouth
LP of the mouth most commonly occurs inside of the cheeks, but can affect the tongue, lips, and gums. Oral LP is more difficult to treat and typically lasts longer than LP on the skin. Fortunately, many cases of LP of the mouth cause minimal problems. About 20% of people who have oral LP also have skin LP.
Oral LP typically appears as patches of fine white lines and dots that usually do not cause problems. Dentists often find them during routine check-ups. More severe forms of oral LP can cause painful sores and ulcers in the mouth. Your dermatologist may have to make sure that the sores are not caused by a yeast or an infection and are not canker sores. Sometimes a biopsy of affected tissue may be needed to confirm a diagnosis.
There have been cases of lichen planus-like allergic reactions to dental materials but they are very rare. Specialized patch testing may be used to pinpoint the allergy; removing dental material may be recommended.
Treatment for LP of the Mouth
There is no known cure for oral LP although there are many treatments that eliminate the pain of sores. When the disease causes no pain or burning, treatment may not be needed. More severe forms of LP – those with pain, burning, redness, blisters, sores, and ulcers – can be treated with a variety of medications, both applied to the sores (topical steroids or Protopic) and taken by mouth (oral). As with any disease of the lining of the mouth, LP can lead to poor dental hygiene and gum disease. Careful daily oral hygiene is very important. Schedule regular visits to the dentist for examinations and cleanings at least twice a year.
Lichen Planus of the Genitals
There may be no problems if it is mild, but red areas or open sores may cause pain, especially with sexual intercourse and needs treatment. There are good treatment options, so do mention genital involvement to your physician.
Nail Involvement
Nail changes have been observed in LP. Only a few fingernails or toenails are usually involved, but occasionally all are affected. Nail changes can occur with or without skin involvement.
Nail changes associated with LP include longitudinal ridging and grooving, splitting, nail thinning, and nail loss. In severe cases, the nail may be temporarily or permanently destroyed.
Scalp Involvement
LP can affect hairy areas such as the scalp in rare cases. This is called lichen planopilaris, and can lead to redness, irritation, and in some cases, permanent hair loss.
What is the Course of Lichen Planus?
Lichen planus is generally not harmful. 85% of skin lichen planus cases resolve within 18 months, but it may persist longer especially when affecting the mouth, genitals, or scalp. As it heals, lichen planus often leaves a dark brown discoloration on the skin, called postinflammatory hyperpigmentation, which can persist for months. If drug-related, discontinuing the drug will usually result in clearing, although the process may take many months.
